Radiotherapy planning
First of all: what is radiotherapy?
Given the premise that certain types of radiation can deal more damage to the DNA of tumor cells than to their healthy counterparts, radiotherapy is the use of radiation, such as photons, electron beams, or protons, to extinguish or shrink tumors while sparing healthy organs as much as possible.
In a nutshell:
Radiotherapy is the art of treating cancer with something that may cause cancer
From the beginning
Once a patient is diagnosed with cancer and referred to radiotherapy treatment, the oncologist often orders a CT scan or occasionally an MRI. These diagnostic tools provide crucial insights into the tumor’s position and geometry.
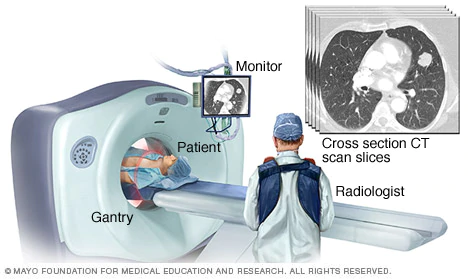
Image taken from the website https://www.mayoclinic.org/tests-procedures/ct-scan/multimedia/ct-scan-slices/img-20008348
With the CT scan in hand the oncologist can now prescribe a radiation dose, measured in Gray, for each organ involved in the treatment. For the tumors, the doctors would like to prescribe a lower bound of dose, while for the critial organs around the tumor, they would prescribe an upper bound of dose.
Linear accelerator
At this point you might wonder, “but how exactly can they deliver this radiation to the patient?” or “where does this radiation come from?” Here is where the engineers and physicists can be proud: they’ve created the linear acelerator! This is an enormous apparatus capable of circumnavigating the patient, delivering radiation from various angles.
The MLC
Nevertheless, as Uncle Ben would say: “with great power comes great responsibility.”
In radiotherapy, the ultimate goal is to direct radiation precisely at the tumor while sparing the patient’s healthy organs.To accomplish this, modern linear accelerators feature a multi-leaf collimator (MLC) – an assembly of collimating blades that dynamically shape the radiation field during treatment, allowing several non-trivial shapes per angle.”
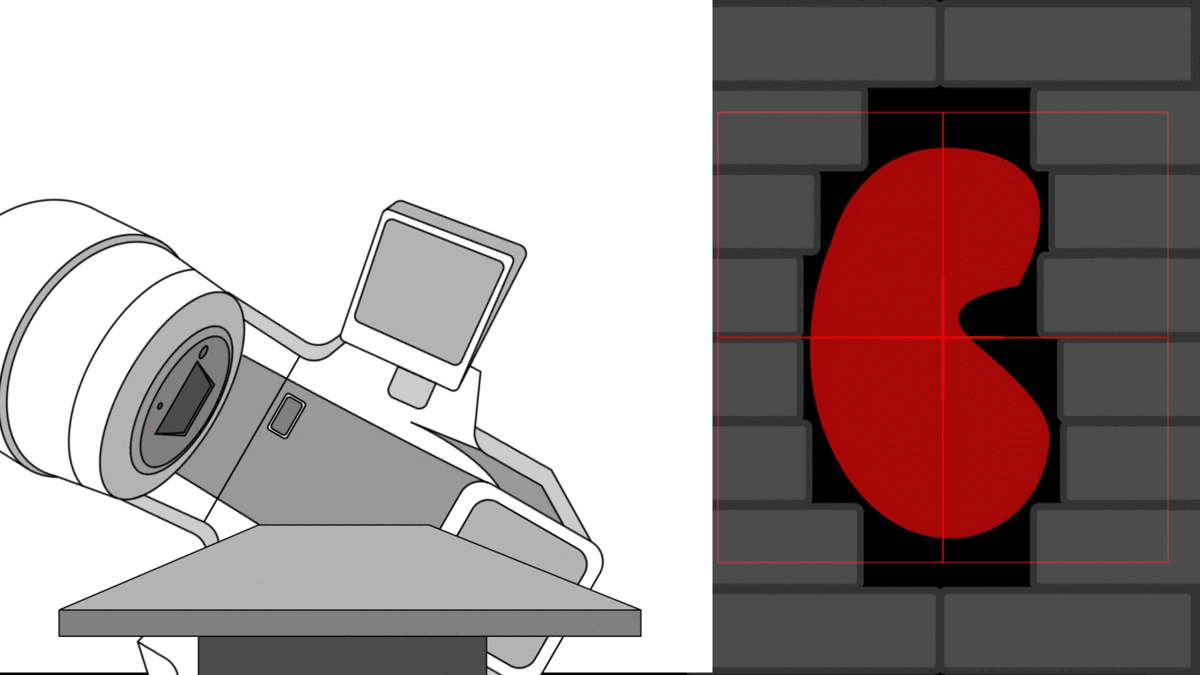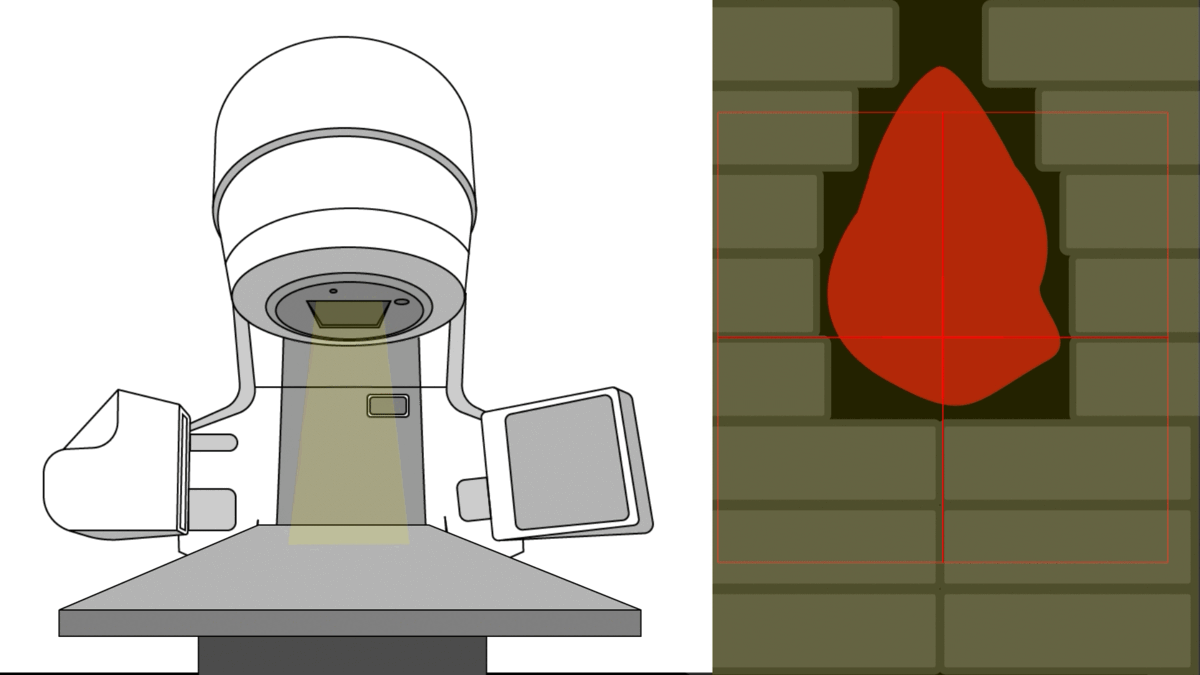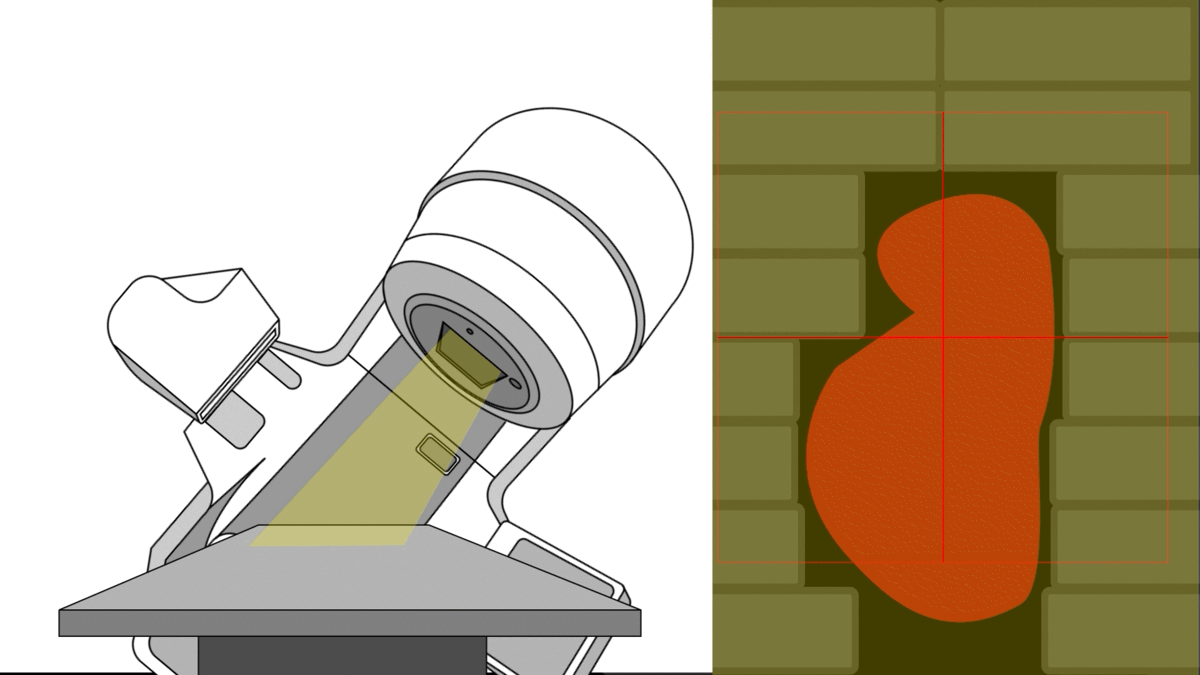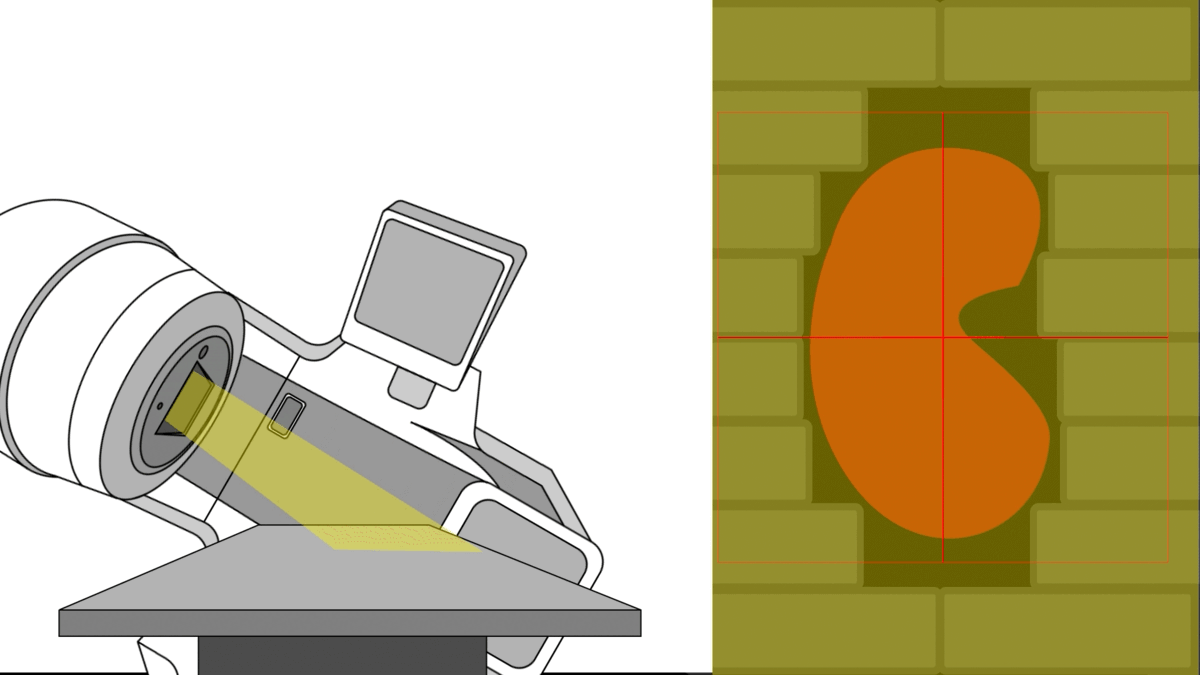
Bear in mind that this is a simple case where the MLC apertures chosen are only matching the tumor's contour.
Planning phase
Finally, with the DICOM data from the CT scan and the prescribed radiation doses, the team of medical physicists must now orchestrate the synergy between the linear accelerator and the MLC to deliver the required dose to the patient. This, ladies and gentlemen, is what is known as radiotherapy planning.
Okay, but where does the optimization come in?
One way of interpreting the dose delivery problem is to minimize the total dose delivered to the patient, subject to the dose prescriptions given by the oncologist. In other words, the goal of the planning phase is to optimize the dose distribution throughout the patient. Which is, of course, what this is all about: optimization!
The prevalent approach for most optimization problems in radiotherapy planning involves discretizing the patient’s organs into voxels through a “3D reconstruction” of the CT scan data and optimizing the dose in every patient’s voxel. The outcome is a tailored suggestion for the radiation dose distribution that will be deposited in the patient’s body within the limitations of the linear accelerator. Luckly, this solution can be visualized in a very nice way:
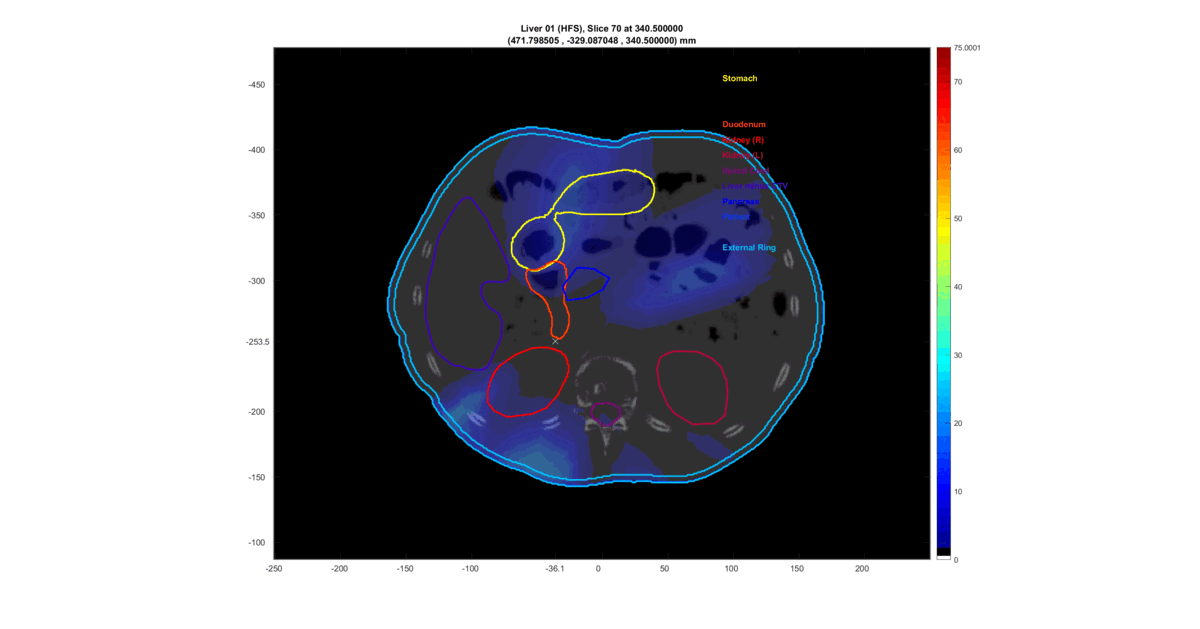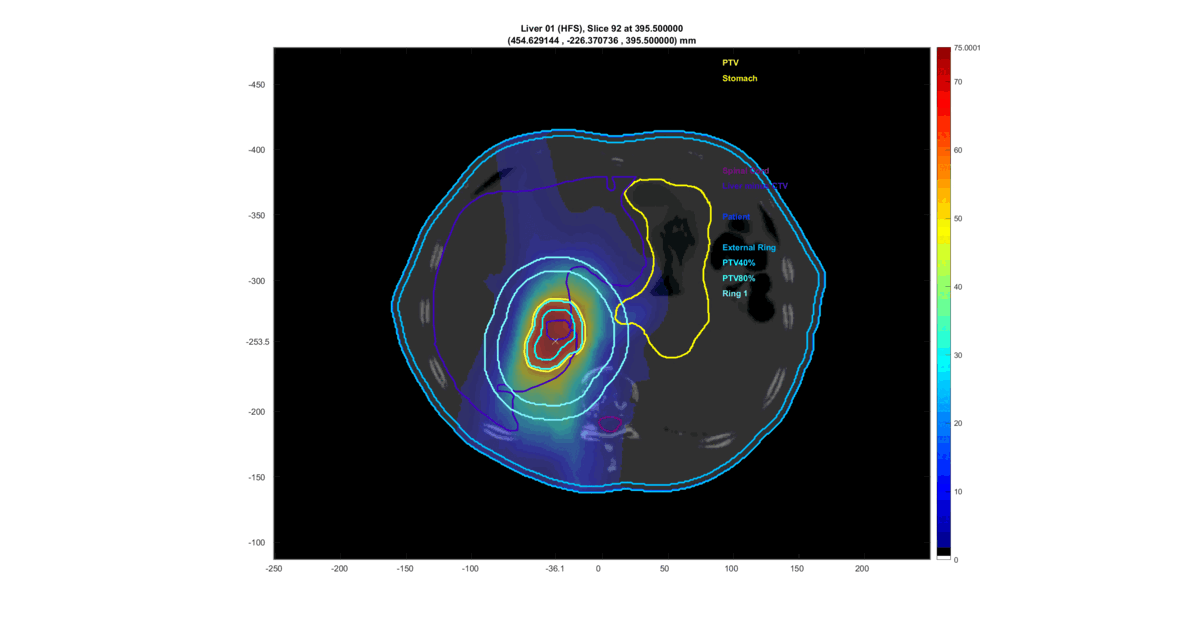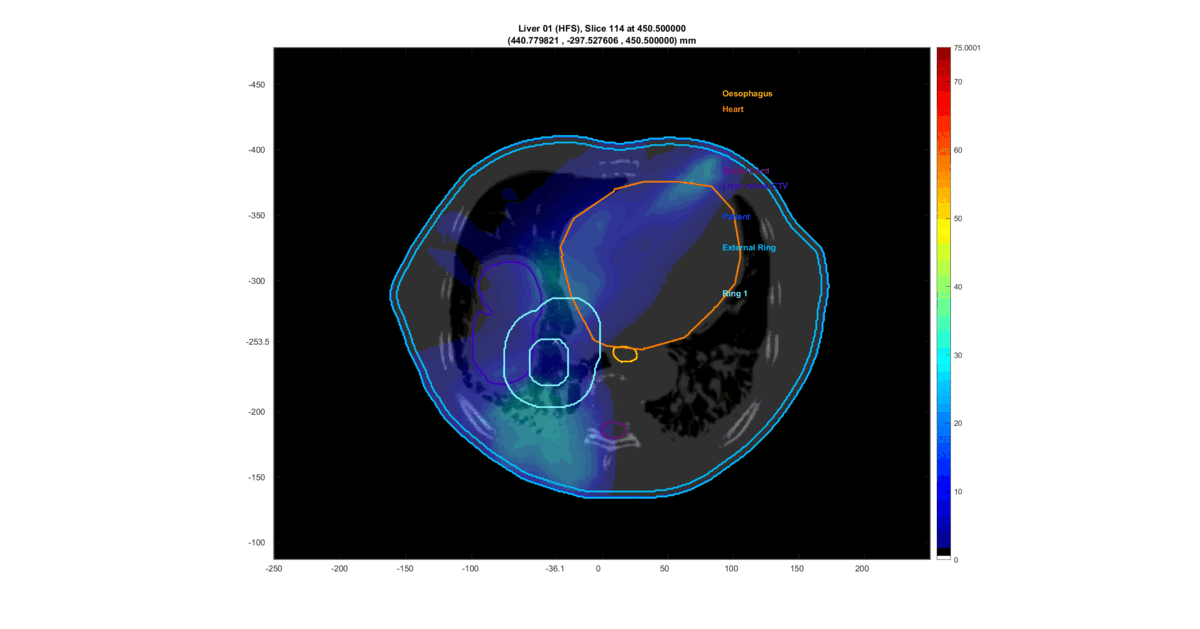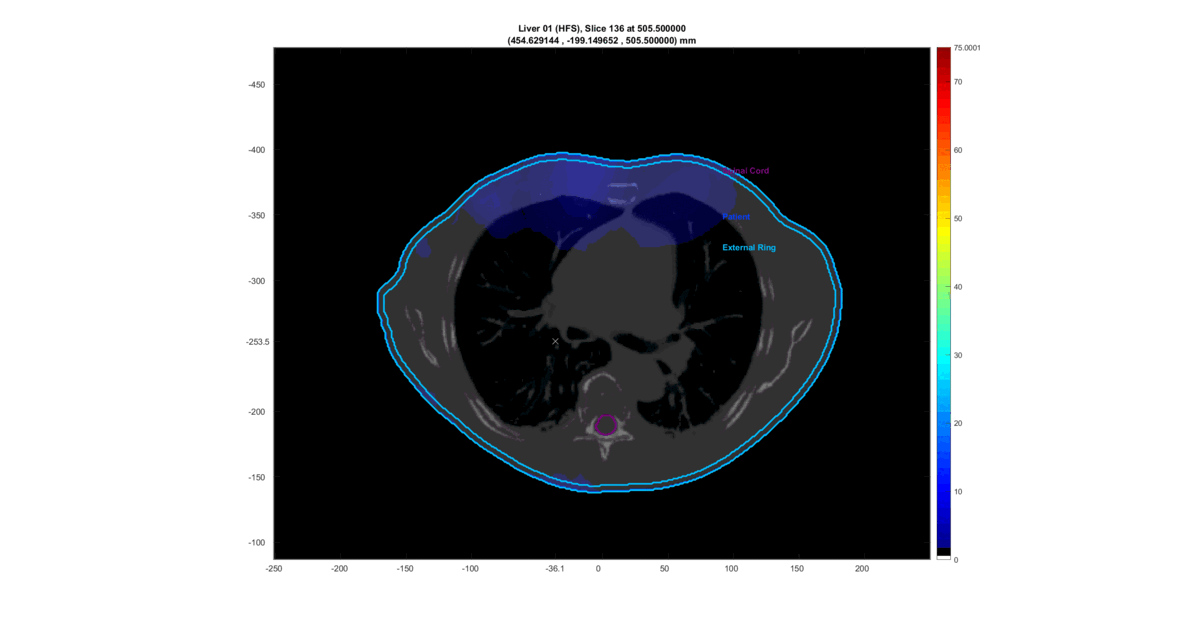
This is a loop through the tomographic slices of the patient with the resultant radiation dose plotted on top.
In closing, for a more in-depth yet still beginner-friendly introduction to this subject, I highly recommend the initial sections of my report “Primal-dual interior point algorithm for the fluence map optimization problem”.
Congratulations for reading this far! I am glad I managed to catch your attention talking about radiotherapy. Feel free to send me an email if you have any questions :)
